The Statistics That Reveal a Crisis:
According to the American Animal Hospital Association (AAHA), 68% of pet owners leave veterinary appointments with unanswered pet health questions. More disturbing: 45% don’t understand their vet’s diagnosis, and 52% admit to ignoring veterinary advice because they didn’t comprehend it.

This communication breakdown costs pet owners approximately $2,000-5,000 annually in preventable disease treatment and reduces pet lifespans by an average of 2.5 years.
The problem isn’t vets or owners—it’s the system. Veterinary appointments average 15-20 minutes, including exam, diagnosis discussion, treatment planning, and billing. Within this compressed timeframe, owners rarely ask the right pet health questions, and vets rarely explain why those pet health questions matter.
This comprehensive guide changes that equation.
“The greatest wealth is health.” — Virgil
This ancient wisdom applies equally to our pets. A preventive healthcare approach—grounded in informed questioning—is the greatest investment you can make in your animal companion’s longevity and quality of life.
Proactive pet care is just a click away! Discover more essential tips on these 9 critical questions to ask at PetCastel today
Q1: What Specific Diseases Should We Screen For Based on My Pet’s Age, Breed, and Genetics?
Why This Question Matters:
This single question determines whether your pet receives reactive care (treating disease after it develops) or preventive care (detecting disease before symptoms appear).
The difference? Caught at stage 1 vs. stage 4 of disease costs 60-70% less and produces dramatically better outcomes.
Breed-Specific Disease Risk (The Genetics Factor):
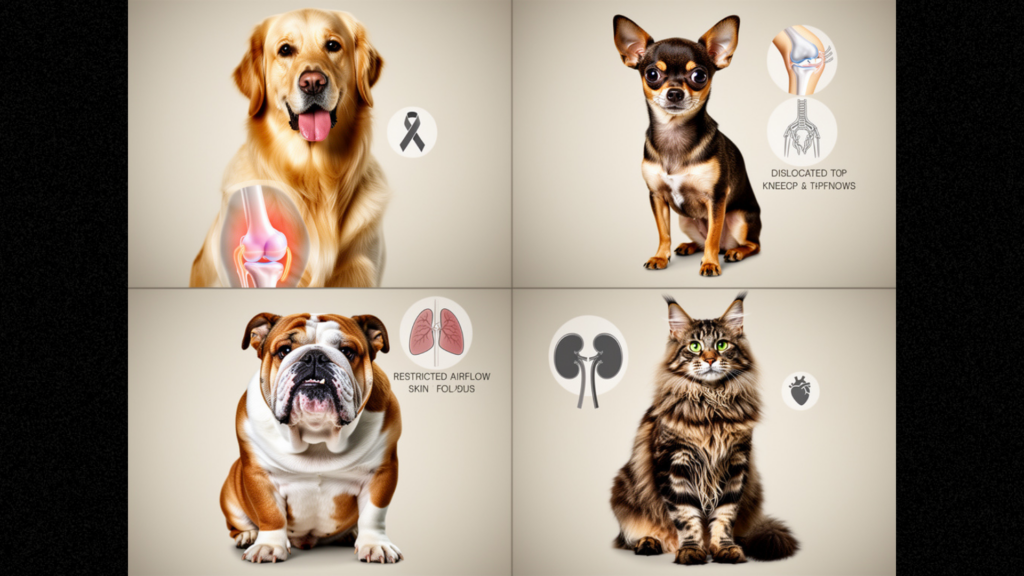
Every breed has inherited predispositions:
- Golden Retrievers: 50% develop hip dysplasia; highest hemangiosarcoma (cancer) rates; DCM (heart disease); cataracts
- Small breeds (Chihuahuas, Yorkies): Patellar luxation (kneecap dislocation); tracheal collapse; early-onset dental disease
- Bulldogs/Pugs: Brachycephalic airway syndrome (breathing problems); skin fold infections; heat intolerance
- Persians: Polycystic kidney disease (PKD); 40% affected; genetic test available
- Maine Coons: Hip dysplasia; spinal muscular atrophy (SMA)
- Cats (general): Hypertrophic cardiomyopathy (HCM); chronic kidney disease (affects 30% of senior cats); diabetes (5-7% of cats)
Age-Related Screening Changes:
Your pet’s screening needs transform with age:
- Puppies/Kittens: Genetic screening, congenital condition detection, parasite monitoring
- Young Adults (1-7 years): Minimal screening; annual physical exam most important
- Mature (7-10 years): Annual bloodwork becomes critical; baseline comparisons essential; cancer surveillance begins
- Senior (10+ years): Twice-yearly exams; twice-yearly bloodwork; ultrasound imaging; blood pressure monitoring
What You Should Hear:
A competent vet will:
- Name specific diseases (not vague “routine screening”)
- Explain prevalence for YOUR pet’s breed
- Justify each test with clinical reasoning
- Distinguish this year vs. future screening
- Provide written timeline and costs
Red Flags:
- “Everything looks normal, so no screening needed” (assumes no symptoms = no disease)
- “Standard bloodwork for all dogs” (ignores breed-specific risks)
- “We’ll wait for symptoms” (reactive, not preventive)
- No mention of your pet’s specific breed predispositions
Q2: Is My Pet at Ideal Weight? What Should They Weigh, and How Will We Monitor Progress?
The Obesity Epidemic:
59.5% of US dogs and 60.5% of US cats are overweight or obese. This isn’t a cosmetic issue—it’s a disease that reduces lifespan by 2.5 years (equivalent to 20% of a dog’s expected life).
“An ounce of prevention is worth a pound of cure.” — Benjamin Franklin
Franklin’s wisdom perfectly encapsulates weight management. Preventing obesity saves years of treating its complications—diabetes, arthritis, heart disease, and cancer.

Why Weight Matters (The Pathophysiology):
Obesity isn’t just extra weight. It’s a metabolic disease causing:
- Diabetes: Obesity causes insulin resistance; 80% of diabetic pets are overweight
- Joint disease: Excess weight accelerates arthritis onset and severity
- Cancer: Obesity promotes tumor growth; higher cancer rates in overweight pets
- Heart disease: Hypertension, cardiovascular strain, reduced exercise tolerance
- Liver disease: Hepatic lipidosis (fatty liver); non-alcoholic fatty liver disease
- Shortened lifespan: Documented 2.5-year reduction
Body Condition Score (BCS) Assessment:
Vets use a standardized 1-9 scale:
| BCS Score | Classification | Physical Characteristics |
|---|---|---|
| 4-5 | Ideal Weight | Ribs easily felt, waist visible from above, abdomen tucked |
| 6-7 | Overweight | Ribs hard to feel, waist barely visible, slight abdominal sag |
| 8-9 | Obese | Ribs not palpable, no waist definition, significant abdominal sag |
Most owners visually assess incorrectly. If you can’t see ribs, the dog is overweight—period.
Critical pet health questions to Ask:
- “What’s my pet’s specific BCS score on the 1-9 scale?”
- “What’s the ideal weight number, and how was it calculated?”
- “What’s realistic weight loss pace?” (Healthy: 1-2% body weight weekly)
- “Should we test thyroid before starting weight loss?” (Hypothyroidism prevents weight loss)
- “What’s the specific daily calorie target?” (Not vague “feed less”)
Implementation:
Ask for written calorie recommendation, portion sizes, treat limits, and exercise plan. Schedule weigh-ins every 4-6 weeks with BCS reassessment.
Q3: Can You Explain My Pet’s Bloodwork Results—What’s Normal, What’s Abnormal, and What It Means?
The Interpretation Gap:

Most owners receive bloodwork reports with values like:
WBC: 7.2 (5.5-16.5)
Thyroid: 1.8 (0.8-3.5)
Kidney: Normal
They assume: “Numbers are in range, so everything’s fine.”
But they have no idea what these values mean, whether slightly low-normal values indicate early disease, or what therapeutic action is needed.
“Knowledge is power.” — Francis Bacon
Understanding your pet’s bloodwork results is perhaps the most empowering knowledge you can possess. It transforms you from a passive recipient of care to an informed partner in your pet’s health management.
Key Bloodwork Values Explained:
| Test Category | Specific Values | What It Indicates |
|---|---|---|
| Complete Blood Count (CBC) | WBC, RBC, Hemoglobin, Platelets | Infection levels, anemia, immune function, clotting ability |
| Chemistry Panel (CMP) | BUN, Creatinine, ALT, AST, Glucose, Electrolytes, Albumin | Kidney/liver function, diabetes, malnutrition, dehydration |
| Thyroid Function | TSH, T4 | Hypothyroidism (affects 10% of middle-aged dogs), metabolism |
Complete Blood Count (CBC):
- WBC: Infection-fighting white blood cells (low = immune suppression; high = infection/leukemia)
- RBC/Hemoglobin: Red cell oxygen-carrying capacity (low = anemia; causes lethargy)
- Platelets: Clotting cells (low = bleeding risk)
Chemistry Panel (CMP):
- Kidney Values (BUN, Creatinine): Early kidney disease detectable 3+ years before symptoms (crucial for senior pets)
- Liver Values (ALT, AST): Liver disease, drug toxicity, hepatitis
- Glucose: Diabetes or hypoglycemia; elevated = pre-diabetes or diabetes
- Electrolytes (Sodium, Potassium): Dehydration, kidney/heart disease
- Albumin: Malnutrition, liver disease, kidney disease
Thyroid Function:
- TSH/T4: Hypothyroidism (most common endocrine disease in dogs; affects 10% of middle-aged dogs)
- Hypothyroidism causes: weight gain (untreatable without hormone replacement), lethargy, coat problems, ear infections
Critical Bloodwork Questions:
- “Which values are abnormal and why?” (Get specific explanations)
- “Do any abnormal values indicate developing disease?” (Not all abnormalities need treatment)
- “What’s the progression if we don’t treat?” (If kidney values slightly elevated, what happens in 1 year, 5 years?)
- “Should we retest in 4 weeks?” (Some values need trending, not one-time assessment)
- “Are any values concerning enough to change treatment?” (Might indicate need for medication adjustment)
Q4: Which Vaccines Does My Pet Actually Need This Year, and Why? Which Are Optional?”
The Vaccination Confusion:
Most owners think vaccines follow a rigid schedule: “All dogs get this vaccine annually.”
Reality is more nuanced. The AAHA guidelines distinguish:
Core Vaccines (recommended for ALL pets):
- Dogs: Rabies, DHPP (distemper, parvovirus)
- Cats: Rabies, FVRCP (feline distemper, calicivirus, rhinotracheitis)
Non-Core Vaccines (based on lifestyle/risk):
- Dogs: Bordetella (kennel cough), Leptospirosis, Lyme disease
- Cats: FeLV (feline leukemia), FIV, rabies (indoor cats: lower priority)
Frequency Matters:
Many vaccines don’t require annual boosters:
| Vaccine Type | Frequency | Clinical Notes |
|---|---|---|
| Rabies | Every 3 years (after initial series) | Core vaccine; legal requirement in most jurisdictions |
| DHPP/FVRCP | Every 3 years for adults | Annual for puppies/kittens initially; titer testing available |
| Bordetella | Annual if high-risk | Only if boarding, dog parks, or shows; lifestyle-dependent |
| Leptospirosis | Annual | Immunity wanes faster; higher outdoor exposure risk |
Ask These pet health questions:
- “Which vaccines are core vs. non-core?” (Core = must have; non-core = lifestyle-dependent)
- “Does my pet really need annual boosters, or can we extend to 3 years?” (Based on titer testing)
- “Which vaccines are necessary given my pet’s lifestyle?” (Indoor cat ≠ outdoor working dog)
- “Are there vaccine reactions I should monitor for?” (Lethargy, vomiting, facial swelling warrant vet call)
- “Can we do titer testing instead of boosters?” (Measures immunity; avoids unnecessary revaccination)
Red Flags:
- Automatically giving all vaccines to all animals annually
- No distinction between core and non-core
- No lifestyle assessment
- “Pets need these vaccines” (lacks individual reasoning)
Q5: What Parasite Prevention Does My Pet Need Year-Round, and Why?”
The Parasite Reality:
Most owners think parasites are eliminated with a treatment or two. Actually:
- Heartworm: Year-round prevention essential; one missed dose = heartworm infection ($1,500-3,000+ treatment)
- Fleas/Ticks: Year-round in most climates; not seasonal anymore due to climate change
- Intestinal Parasites: Hookworms, roundworms, whipworms; transmissible to humans
Geographic Variation:
Parasite risk differs dramatically by location:
- Southern US: Year-round heartworm, fleas, ticks
- Northern US: Winter break possible for some parasites, but heartworm prevention still needed
- Coastal areas: Higher intestinal parasite risk
- Your specific zip code: Affects recommendations
Specific Questions:
- “Is my pet on heartworm prevention, and should it be year-round?” (Yes, year-round in most areas)
- “Does the prevention also cover fleas and ticks?” (Many modern meds do; simplifies compliance)
- “Should we test for heartworm?” (Annual test important; missed infection is emergency)
- “What’s my pet’s intestinal parasite risk?” (Indoor cat = lower risk; outdoor dog = higher risk)
- “Are there any fecal exams recommended?” (Annual fecal exam recommended for outdoor pets)
Prevention Options:
Modern options include:
- Oral medications: Monthly (Simparica, NexGard) or quarterly/yearly (Credelio)
- Topical: Monthly application (Advantage II, Revolution)
- Injectable: 6-month heartworm prevention (ProHeart 6)
- Collars: Extended flea/tick prevention (Seresto)
Each has advantages/disadvantages; choice depends on pet compliance, lifestyle, and owner preference.
Dental disease can silently harm your pet’s health. Explore comprehensive prevention strategies and caring advice at PetCastle.me now! Get the guide
Q6: How Is My Pet’s Dental Health? Do They Need Professional Cleaning? What Will Happen If We Don’t Address Dental Disease?
The Dental Epidemic:
80% of dogs and 90% of cats over age 3 have dental disease. Yet only 10% of pet owners pursue professional cleaning, treating dental disease as cosmetic rather than critical.
“A smile is the best cosmetic, but healthy teeth are what create that smile.” — Dr. Jack Canfield, veterinary advocate
This wisdom reminds us that dental health isn’t vanity—it’s fundamental to quality of life and systemic health.
Why Dental Disease Matters (The Systemic Impact):
Dental disease isn’t just about bad breath. Bacteria enter the bloodstream through diseased gums, causing:
- Kidney disease: Bacteria seed kidneys; chronic kidney disease risk increases with untreated dental disease
- Heart disease: Endocarditis (heart valve infection) from oral bacteria; can be fatal
- Liver disease: Liver infection from chronic bacteremia
- Pain: Tooth decay, abscesses, loose teeth cause chronic pain (often misattributed to aging)
- Behavioral changes: Pets with tooth pain become aggressive, withdrawn, or anxious
Dental Assessment:
During checkup, vet should examine:
- Plaque/tartar buildup (visible yellow/brown on teeth)
- Gum inflammation/redness
- Tooth mobility (loose teeth = advanced disease)
- Oral odor (severe indicates infection)
- Stage of disease (1-4 scale)
Professional Cleaning Reality:
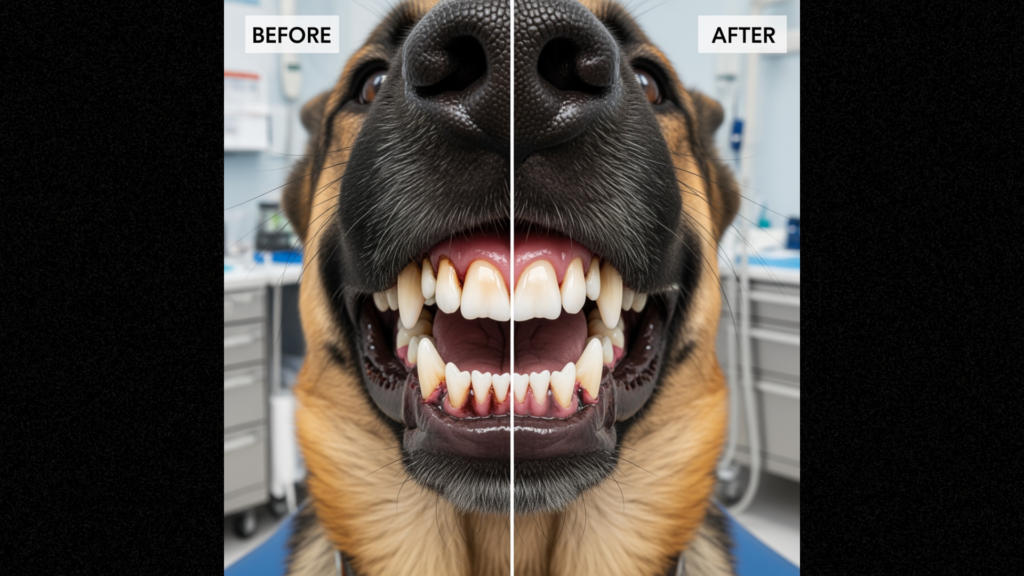
Many owners hesitate due to anesthesia concerns (“Why put them under for teeth cleaning?”).
Important context:
- Anesthesia is necessary: Manual scaling without anesthesia is inhumane (like dentistry without numbing)
- Modern anesthesia is safe: Pre-anesthesia bloodwork identifies risks; most pets handle cleaning safely
- Cost vs. benefit: $400-1,500 cleaning ≪ $5,000+ treatment of systemic disease from untreated dental disease
- Lifespan impact: Treated dental disease = improved quality of life, fewer systemic infections
Critical Questions:
- “What stage is my pet’s dental disease on the 1-4 scale?”
- “Does my pet need professional cleaning now or can we wait?”
- “If we don’t treat, what will happen?” (Forces owner to understand consequences)
- “How long does the procedure take, and how is anesthesia monitored?”
- “What’s the cost breakdown?” (Cleaning, extractions, medications, monitoring)
- “What home care can I do?” (Brushing, dental diet, water additives)
Q7: Are There Any Medications My Pet Is Taking That Need Dose Adjustment or Monitoring?
The Adjustment Gap:
Many pets are on chronic medications (thyroid, heart medication, pain management) that require periodic adjustment based on:
- Weight changes: 10-pound weight loss may require thyroid dose reduction
- Age changes: Senior pets may need medication adjustments
- Disease progression: If initial treatment dose ineffective, dosing may need increase
- New health issues: New diagnosis may interact with existing medications
Yet many owners continue original doses indefinitely, leading to:
- Underdose: Insufficient disease control (unmanaged pain, uncontrolled thyroid)
- Overdose: Toxicity, side effects (excessive thirst/urination, tremors)
Questions to Ask:
- “Has my pet’s thyroid medication been adjusted based on recheck TSH levels?” (Hypothyroid dogs often need dose adjustment after 4-6 weeks)
- “Are there any monitoring requirements for this medication?” (Some drugs require annual bloodwork to check organ function)
- “What side effects should I watch for?” (Many side effects go unreported because owners don’t know they’re related to meds)
- “Should we recheck medication effectiveness?” (Timelines: thyroid after 4-6 weeks of starting/adjusting; heart meds after 2 weeks; pain meds weekly initially)
- “Are there any medication interactions I should know about?” (New supplements or medications can interact)
“The best doctor gives the least medicines.” — Benjamin Franklin
The same principle that applies to human medicine also holds true for veterinary care: medication adjustments should be based on clinical need, not habit. Regular monitoring ensures therapeutic efficacy while avoiding unnecessary dosing. This approach helps ensure pets receive appropriate treatment without exposure to excess pharmaceuticals. Working closely with your veterinarian to review treatment plans leads to safer and more effective healthcare for your animal companions.
Q8: Are There Any Behavioral or Lifestyle Changes I Should Know About That Might Indicate Health Issues?
Why This Question Matters:
Many health problems manifest as behavioral changes attributed to “aging” or “just how they are”:
- Aggression: Often pain-related (arthritis, ear infections, dental disease)
- Lethargy: Not normal aging; indicates thyroid disease, pain, depression, or systemic disease
- Litter box avoidance (cats): Often indicates pain (arthritis, urinary issues), not behavioral problem
- House soiling: May indicate medical issue (kidney disease, diabetes, incontinence) not behavioral
- Anxiety/nervousness: Could be pain-related or indicate thyroid/metabolic disease
- Sleep changes: Excessive sleeping might indicate depression or disease
Specific Questions:
- “Are there any behavioral changes you’re noticing at home?” (Ask owner first; they know pet best)
- “Have my pet’s eating or drinking habits changed?” (Increased thirst = diabetes, kidney disease; decreased appetite = pain or nausea)
- “Is my pet having accidents in the house?” (Medical vs. behavioral distinction critical)
- “Have you noticed any mobility issues—limping, stiffness, reluctance to jump?” (Pain assessment)
- “Is my pet sleeping more than usual?” (Normal variation vs. lethargy indicating disease)
Q9: Should We Discuss Emergency Care Planning and What Expenses I Should Expect?
The Financial Reality:
Emergency vet visits cost $800-2,000+ per visit. Most owners don’t budget for this reality:
| Emergency Condition | Typical Cost Range | Why It’s Expensive |
|---|---|---|
| Urinary obstruction (cat) | $2,000-5,000 | Requires catheterization, hospitalization, medications, monitoring |
| Bloat/gastric dilation (dog) | $3,000-5,000 | Emergency surgery, anesthesia, intensive post-op care required |
| Hit by car trauma | $5,000-15,000+ | X-rays, surgery, blood transfusions, ICU monitoring possible |
Planning Questions:
- “What should I do if an emergency happens after hours?” (Know your emergency clinic location, hours, phone number)
- “What’s typically the most expensive emergency for my pet’s breed?” (Breed-specific knowledge helps prepare)
- “Should I consider pet insurance?” (Recoup 70-90% of costs; evaluate ROI based on age/breed)
- “What’s your payment plan if I can’t pay upfront?” (Some clinics offer financing)
- “Should we discuss quality-of-life end-of-life planning now?” (For senior pets, clarity helps later decisions)
PRACTICAL IMPLEMENTATION
Before Your Appointment:
- Write down all pet health questions (don’t rely on memory; stress affects retention)
- Note any behavioral changes, appetite changes, or health concerns
- Bring list of current medications
- Bring previous medical records if first visit with this vet
During Appointment:
- Ask vet to physically show you what they’re assessing (weight, teeth, ears)
- Request written explanations of abnormal findings
- Ask for specific numbers/timelines (not vague “keep an eye on it”)
- Take photos of written recommendations
Leave With:
- Written list of recommendations with timelines and costs
- Specific medication doses and adjustment schedule
- Next appointment scheduled for follow-ups
- Contact number for questions that arise after appointment
CONCLUSION
“The bond with a true dog is as deep as the bond can get.” — J.R.R. Tolkien
That bond deepens when we take responsibility for our pets’ health through informed questioning and proactive care. The 9 pet health questions in this guide represent your commitment to that bond.
Ultimately, better outcomes in pet healthcare begin with informed pet owners who ask thoughtful pet health questions and engage in clear veterinary communication. Understanding veterinary bloodwork interpretation and understanding pet bloodwork supports early disease detection pets depend on for longer, healthier lives.
Focusing on preventive pet care, vaccine needs for pets, parasite prevention for pets, and pet dental health helps control pet healthcare costs while improving pet longevity and quality of life. Awareness of breed-specific pet diseases, pet weight management, obesity in dogs and cats, chronic pet medication, and pet behavioral health changes enables proactive pet care strategies that reduce emergency pet care costs.
Through ongoing pet owner education, families can make confident decisions that protect their pets’ health, comfort, and well-being for years to come.
Ready to give your pet the longest, healthiest life? Visit PetCastle.me to dive deeper into these lifesaving questions and connect with a community dedicated to informed, proactive pet care. Start your journey today Explore More.
Remember: A pet that receives preventive, informed care can live 2.5 years longer on average. That’s 2.5 additional years of companionship, love, and shared moments. That’s worth every question you ask.
FAQs
1. Why does my veterinarian recommend bloodwork for my healthy pet?
Routine testing is a pillar of Preventive Pet Care. By utilizing Proactive Pet Care Strategies, your vet can achieve Early Disease Detection Pets, catching internal issues before symptoms arise and ensuring your pet remains a healthy, active participant in life.
2. How can I learn to read my dog or cat’s lab report?
Mastering Veterinary Bloodwork Interpretation and Understanding Pet Bloodwork is empowering knowledge. Through clear Veterinary Communication, Informed Pet Owners can learn how CBC and Chemistry values reflect their pet’s internal stability.
3. What are the signs that my pet needs immediate blood testing?
Sudden Pet Behavioral Health Changes or shifts in appetite require investigation. Testing is vital for Pet Weight Management, especially since Obesity in Dogs and Cats can mask issues, or when monitoring for known Breed-Specific Pet Diseases.
4. What is the difference between a CBC and a Blood Chemistry Panel?
The CBC checks blood cells, which helps determine Vaccine Needs for Pets and the efficacy of Parasite Prevention for Pets. The Chemistry Panel monitors organ function, which is essential for maintaining Pet Longevity and Quality of Life.
5. How much does pet bloodwork usually cost?
While Pet Healthcare Costs vary, bloodwork is an investment that prevents high Emergency Pet Care Costs later. It is a clinical necessity for pets requiring Pet Dental Health procedures or those managed with Chronic Pet Medication.
